CETRAPIB
1 EVACETRAPIB
2 TORCETRAPIB
3
4

1 EVACETRAPIB


with
 Evacetrapib
Evacetrapib

 THE ESTER OF EVACETRAPIB
THE ESTER OF EVACETRAPIB




1 EVACETRAPIB
2 TORCETRAPIB
3
4

1 EVACETRAPIB

Evacetrapib, LY2484595
Evacetrapib is an experimental drug being investigated to raise high-density lipoprotein cholesterol (HDL-C) via inhibition of the cholesteryl ester transfer protein (CETP)
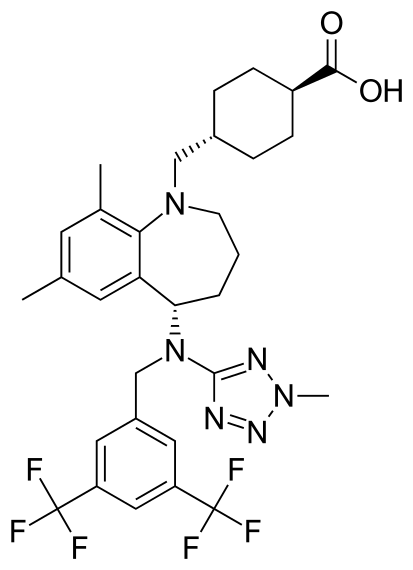
Trans-4-({(5S)-5-[{[3,5-bis(trifluoromethyl)phenyl]methyl}(2-methyl-2H-tetrazol-5- yl)amino]-7,9-dimethyl-2,3,4,5-tetrahydro-1H-benzazepin-1-yl}methyl) cyclohexanecarboxylic acid
trans-4-[[(5S)-5-[[[3 ,5- bis(trifluoromethyl)phenyl]methyl] (2-methyl-2H-tetrazol-5-yl)amino]-2, 3,4,5- tetrahydro-7,9-dimethyl- IH- 1 -benzazepin- 1 -yl]methyl]-cyclohexanecarboxylic acid
trans-4-[5(S)-[N-[3,5-Bis(trifluoromethyl)benzyl]-N-(2-methyl-2H-tetrazol-5-yl)amino]-7,9-dimethyl-2,3,4,5-tetrahydro-1H-1-benzazepin-1-ylmethyl]cyclohexanecarboxylic acid
1186486-62-3 is cas
UNII-51XWV9K850
- C31-H36-F6-N6-O2
- 638.6534
- lily……….. .innovator
Evacetrapib is a drug under development by Eli Lilly & Company (investigational name LY2484595) that inhibits cholesterylester transfer protein, which transfers and thereby increases high-density lipoprotein and lowers low-density lipoprotein. It is thought that modifying lipoprotein levels modifies the risk of cardiovascular disease.[1]
The first CETP inhibitor, torcetrapib, was unsuccessful because it increased levels of the hormone aldosterone and increased blood pressure,[2] which led to excess cardiac events when it was studied.[2] Evacetrapib does not have the same effect.[1] When studied in a small clinical trial in people with elevated LDL and low HDL, significant improvements were noted in their lipid profile.[3]
LY-2484595 is in phase III clinical trials at Lilly for the treatment of high-risk vascular disease and in phase II for the treatment of dyslipidemia.
Evacetrapib is one of two CETP inhibitors currently being evaluated (the other being anacetrapib).[1] Two other CETP inhibitors (torcetrapib and dalcetrapib) were discontinued during trials due to increased deaths and little identifiable cardiovascular benefit (despite substantial increases in HDL). Some hypothesize that CETP inhibitors may still be useful in the treatment of dyslipidemia, though significant caution is warranted.[2]

……………………………..
Intermediate Preparation Scheme 1
Scheme 5

Scheme 7
…………………
trans-4-[[(5S)-5-[[[3 ,5- bis(trifluoromethyl)phenyl]methyl] (2-methyl-2H-tetrazol-5-yl)amino]-2, 3,4,5- tetrahydro-7,9-dimethyl- IH- 1 -benzazepin- 1 -yl]methyl]-cyclohexanecarboxylic acid, (identified according to its Chemical Abstracts Index Name (referred to herein as BCCA) having the structure of Formula I illustrated below, and pharmaceutically acceptable salts of this compound.
I
The compound, BCCA, can be a free acid (referred to herein as BCCA free acid), or a pharmaceutically acceptable salt thereof, as a solvate (referred herein as BCCA’solvate) and a hydrate (referred to herein as BCCA ‘hydrate). The solvate molecules include water (as the hydrate), methanol, ethanol, formic acid, acetic acid, and isopropanol.
Scheme 1
(MeO) SO
Scheme 2
Scheme 3 : Alternate method for preparing BCCA
Preparation 11 Preparation 12
Preparation 13 Preparation 14 Preparation 15
Preparation 16
Preparation 17
Example 16
Scheme 4
………….
formula III below
with
Preparation 10 (Trans)-methyl 4-(((S)-5-((3,5-bis(trifluoromethyl)benzyl)(2-methyl-2H-tetrazol-5-yl)amino)-7,9-dimethyl-2,3,4,5-tetrahydro-1H-benzo[b]azepin-1-yl)methyl)cyclohexanecarboxylate (12)
Charge a flask equipped with an overhead stirrer, temperature probe, nitrogen inlet with (S)—N-(3,5-bis(trifluoromethyl)benzyl)-7,9-dimethyl-N-(2-methyl-2H-tetrazol-5-yl)-2,3,4,5-tetrahydro-1H-benzo[b]azepin-5-amine (5 g, 10.03 mmoles) and sodium triacetoxyborohydride (3.19 g, 15.05 mmoles) and acetonitrile (40 mL). Immerse the flask in an ice bath to cool the slurry to below about 5° C., then add (trans)-methyl 4-formylcyclohexanecarboxylate (2.99 g, 17.57 mmoles, prepared essentially according to the procedures in Houpis, I. N. et al, Tetrahedron Let. 1993, 34(16), 2593-2596 and JP49048639) dissolved in THF (10 mL) via a syringe while maintaining the reaction mixture at or below about 5° C. Allow the reaction to warm to RT and stir overnight. Add NH4Cl (25 mL, 50% saturated aqueous solution) and separate the aqueous layer from the organic layer. The pH of the organic layer should be about 5.5. Warm the organic layer to about 45° C. and add water (16 mL). Add a seed crystal of the titled compound and cool to about 35° C. Collect the resulting solid by filtration and rinse with ACN. Dry to provide 5.80 g of the title compound.
………….


…………………….paper
 THE ESTER OF EVACETRAPIB
THE ESTER OF EVACETRAPIBDevelopment of a Hydrogenative Reductive Amination for the Synthesis of Evacetrapib: Unexpected Benefits of Water
Michael O. Frederick, Scott A. Frank, Jeffrey T. Vicenzi, Michael E. LeTourneau, K. Derek Berglund, Adler W. Edward, and Charles A. Alt
organic process research and development
pp 546–551
Publication Date (Web): March 18, 2014 (Communication)
DOI: 10.1021/op500025v
For the synthesis of cholesteryl ester transfer protein (CETP) inhibitor evacetrapib, a hydrogenative reductive amination was chosen to join the substituted cyclohexyl subunit to the benzazepine core. The addition of water, which suppressed undesired epimerization without affecting the rate of product formation, was key to the reaction’s success. The process was scaled to produce more than 1100 kg of material.

Scheme 1. Synthesis of evacetrapib (5) via a STAB-mediated reductive amination.
aReagents and conditions: a) Na2CO3 (3.0 equiv), toluene, water, 25 °C, 3 h, 98% yield, 99.8:0.2 anti:syn; b) 3 (1.5 equiv), NaBH(OAc)3 (1.5 equiv), ACN, toluene, −10 °C, 2.5 h, 88% yield, 99.2:0.8 anti:syn; c) NaOH (3.0 equiv), water, IPA, 60 °C, 7 h, 92% yield, 99.5:0.5 anti:syn.
References
- Cao G, Beyer TP, Zhang Y, et al. (December 2011). “Evacetrapib is a novel, potent, and selective inhibitor of cholesteryl ester transfer protein that elevates HDL cholesterol without inducing aldosterone or increasing blood pressure”. J. Lipid Res. 52 (12): 2169–76.doi:10.1194/jlr.M018069. PMID 21957197.
- Joy T, Hegele RA (July 2009). “The end of the road for CETP inhibitors after torcetrapib?”. Curr. Opin. Cardiol. 24 (4): 364–71.doi:10.1097/HCO.0b013e32832ac166. PMID 19522058.
- Nicholls SJ, Brewer HB, Kastelein JJ, Krueger KA, Wang MD, Shao M, Hu B, McErlean E, Nissen SE (2011). “Effects of the CETP inhibitor evacetrapib administered as monotherapy or in combination with statins on HDL and LDL cholesterol”. JAMA 306 (19): 2099–109.doi:10.1001/jama.2011.1649.

/////////////////////////
2 TORCETRAPIB
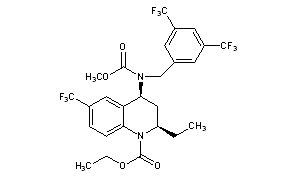









2 TORCETRAPIB

Torcetrapib
CAS : 262352-17-0
(2R,4S)-4-[[[3,5-Bis(trifluoromethyl)phenyl]methyl](methoxycarbonyl)amino]-2-ethyl-3,4-dihydro-6-(trifluoromethyl)-1(2H)-quinolinecarboxylic acid ethyl ester
(2R,4S)-4-[(3,5-bis-trifluoromethylbenzyl)methoxycarbonylamino]-2-ethyl-6-trifluoromethyl-3,4-dihydro-2H-quinoline-1-carboxylic acid ethyl ester
Manufacturers’ Codes: CP-529414
Molecular Formula: C26H25F9N2O4
Molecular Weight: 600.47
Percent Composition: C 52.01%, H 4.20%, F 28.48%, N 4.67%, O 10.66%
Properties: Anhydrous, non-hygroscopic crystals, mp 89-90°. d 1.406.
Melting point: mp 89-90°
Density: d 1.406

Derivative Type: Ethanolate
CAS Registry Number: 343798-00-5
Molecular Formula: C26H25F9N2O4.C2H6O
Molecular Weight: 646.54
Percent Composition: C 52.02%, H 4.83%, F 26.45%, N 4.33%, O 12.37%
Properties: White crystalline powder, mp 54-58°. [a]D -93.3° (c = 1.08 in methanol). d 1.402. Non-hygroscopic. Higher aqueous soly than anhydrous form.
Melting point: mp 54-58°
Optical Rotation: [a]D -93.3° (c = 1.08 in methanol)
Density: d 1.402
Therap-Cat: Antilipemic; antiatherosclerotic.

Torcetrapib (CP-529,414, Pfizer) was a drug being developed to treathypercholesterolemia (elevated cholesterol levels) and prevent cardiovascular disease. Its development was halted in 2006 when phase III studies showed excessive all-cause mortality in the treatment group receiving a combination ofatorvastatin (Lipitor) and torcetrapib.

Medical uses
Torcetrapib has not been found to affect either cardiovascular disease or risk of death in those already taking a statin.[1]
Mechanism
Torcetrapib acts (as a CETP inhibitor) by inhibiting cholesterylester transfer protein (CETP), which normally transfers cholesterol from HDL cholesterol tovery low density or low density lipoproteins (VLDL or LDL). Inhibition of this process results in higher HDL levels (the “good” cholesterol-containing particle) and reduces LDL levels (the “bad” cholesterol).
Development
The first step in the synthesis was a recently created reaction of amination top-chlorotrifluoryltoluene, a reaction that was created by Dr. Stephen Buchwald at MIT.[2]
Development of the drug began around 1990; it was first administered in humans in 1999, and manufacturing at production scale began in Ireland in 2005.[3]
Pfizer had previously announced that torcetrapib would be sold in combination with Pfizer’s statin, atorvastatin (Lipitor); however, following media and physician criticism, Pfizer had subsequently planned for torcetrapib to be sold independently of Lipitor.[4]
Clinical trials
A 2004 trial (19 subjects, non-randomised) showed that torcetrapib could increase HDL and lower LDL with and without an added statin.[5]
Early termination of study
On December 2, 2006 Pfizer cut off torcetrapib’s phase III trial because of “an imbalance of mortality and cardiovascular events” associated with its use.[16]This was a sudden and unexpected event and as late as November 30, 2006Jeff Kindler, Pfizer’s chief executive, was quoted, “This will be one of the most important compounds of our generation.”[16] In the terminated trial, a 60% increase in deaths was observed among patients taking torcetrapib and atorvastatin versus taking atorvastatin alone.[17] Pfizer recommended that all patients stop taking the drug immediately.[18]
Six studies were terminated early.[6] One of the completed studies found it raised systolic blood pressure and concluded “Torcetrapib showed no clinical benefit in this or other studies, and will not be developed further.”[19]
The drug cost $800m+ to bring into Phase III development.[20]

Dec. 2, 2006, was a day drugmakers won’t soon forget. On that day, Pfizer, the world’s biggest drug company, faced devastating news: Its highest profile drug candidate, the cholesterol-targeted molecule torcetrapib, had increased the risk of death in a 15,000-patient clinical trial. In light of the data, Pfizer promptly pulled the plug on the cholesteryl ester transfer protein (CETP) inhibitor that already had cost more than $800 million to develop. The torcetrapib news rocked the cardiovascular research field and left Pfizer without a potential new medication to supplement the blockbuster cholesterol drug Lipitor (atorvastatin), which was careening toward the patent cliff.


……………………

| A Concise Asymmetric Synthesis of Torcetrapib�, M. Guino, P. H. Phua, J-C. Caille and K. K. Hii, J. Org. Chem., 2007, 72, 6290-6293.doi:10.1021/jo071031gAbstract: Optically active torcetrapib was synthesized in seven steps from achiral precursors without the need for protecting groups, utilizing an enantioselective aza-Michael reaction to achieve asymmetry. |

SYNTHESIS………http://pubs.acs.org/doi/suppl/10.1021/jo071031g/suppl_file/jo071031gsi20070612_085123.pdf
………………………..
PATENT
Example 9 Anhydrous, (-)-(2R,4S)-4-[(3,5-Bιs-trιfluoromethyl-benzyl)-methoxycarbonyl-amιnol-2- ethyl-6-trιfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 -carboxylic acid ethyl ester.
A 2.6g portion of 4(S)-[(3,5-bιs-tπfluoromethyl-benzyl)-methoxycarbonyl-amιno]-2(R)- ethyl-6-tπfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 -carboxylic acid ethyl ester (a mixture of predominantly amorphous material with traces of ethanolate crystalline form; the title compound was also prepared in an analogous manner starting from pure amorphous or pure ethanolate material) was charged to 13 milliliters of hexanes and heated to effect a solution at about 60°C The heat was removed and the reaction was allowed to cool to ambient over a one hour period The reaction was seeded with anhydrous (-)-(2R,4S)-4-[(3,5-bιs-tπfluoromethyl-benzyl)- methoxycarbonyl-amιno]-2-ethyl-6-trιfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 – carboxylic acid ethyl ester and granulated for eighteen hours under ambient conditions. Alternately, the anhydrous crystals may be prepared from hexanes without seeding. The product was collected by filtration and air dried. The isolated product X-ray pattern matched the calculated powder pattern. Density: 1.406 Crystal System: Trigonal
Microscopy: Well formed rods and equant (fractured rods) crystals demonstrating high birefringence when viewed across the C axis. Being in the Trigonal crystal system the crystals do not demonstrate birefringence when viewed down the C axis. The crystals demonstrate a cleavage plane perpendicular to the C axis Fusion Microsocopy In Type A oil dissolution at 50°C.
Dry — clear melt at 86°C.
NMR: No trace of ethanolate
Degree of crystallmity: Highly crystalline Hygroscopicity. Non-hygroscopic at 100% relative humidity over 48 hours.
Appearance: Free flowing white powder

Lit References:
Cholesteryl ester transfer protein (CETP) inhibitor. Prepn: M. P. DeNinno et al.,WO 0017164; eidem, US6197786 (2000, 2001 both to Pfizer); of crystalline forms: D. J. M. Allen et al., WO 0140190 (2001 to Pfizer).
Mechanism of action study: R. W. Clark et al., J. Lipid Res. 47, 537 (2006).
Clinical evaluation of effects on HDL cholesterol levels: R. W. Clark et al.,Arterioscler. Thromb. Vasc. Biol. 24, 490 (2004); M. E. Brousseau et al., N. Engl. J. Med. 350, 1505 (2004).
Review of clinical development in combination with atorvastatin: J. R. Burnett,Curr. Opin. Invest. Drugs 6, 944-950 (2005).
References
- Clark, RW; Sutfin TA, Ruggeri RB, Willauer AT, Sugarman ED, Magnus-Aryitey G, Cosgrove PG, Sand TM, Wester RT, Williams JA, Perlman ME, Bamberger MJ (January 22, 2004). “Raising high-density lipoprotein in humans through inhibition of cholesteryl ester transfer protein: an initial multidose study of torcetrapib”. Arteriosclerosis, Thrombosis, and Vascular Biology 24 (3): 490–497.doi:10.1161/01.ATV.0000118278.21719.17. PMID 14739125. Retrieved 2006-12-03.
- Clark, RW; Ruggeri RB; Cunningham D; Bamberger MJ (March 2006).“Description of the torcetrapib series of cholesteryl ester transfer protein inhibitors, including mechanism of action”. Journal of Lipid Research 47(3): 537–552. doi:10.1194/jlr.M500349-JLR200. PMID 16326978. Retrieved 2006-12-03.
- Davidson, MH; McKenny JM; Shear CL; Revkin JH (November 7, 2006).“Efficacy and safety of torcetrapib, a novel cholesteryl ester transfer protein inhibitor, in individuals with below-average high-density lipoprotein cholesterol levels”. Journal of the American College of Cardiology 48 (9): 1774–1781.doi:10.1016/j.jacc.2006.06.067.PMID 17084249. Retrieved 2006-12-03.
- McKenny, JM; Davidson MH; Shear CL; Revkin JH (November 7, 2006).“Efficacy and safety of torcetrapib, a novel cholesteryl ester transfer protein inhibitor, in individuals with below-average high-density lipoprotein cholesterol levels on a background of atorvastatin”. Journal of the American College of Cardiology 48 (9): 1782–1790.doi:10.1016/j.jacc.2006.06.066. PMID 17084250. Retrieved 2006-12-03.
Notes
- Keene, D; Price, C; Shun-Shin, MJ; Francis, DP (Jul 18, 2014). “Effect on cardiovascular risk of high density lipoprotein targeted drug treatments niacin, fibrates, and CETP inhibitors: meta-analysis of randomised controlled trials including 117,411 patients.”. BMJ (Clinical research ed.) 349: g4379. PMID 25038074.
- Buchwald, Stephen (July 23, 2004). “Research Projects”. Retrieved 2007-10-04.
- “Pfizer Begins Production at Torcetrapib/Atorvastatin Manufacturing Facility” (Press release). Pfizer. June 22, 2005. Retrieved 2006-12-03.
- Berenson, Alex (July 26, 2006). “Heart Pill to Be Sold by Itself”. Business(The New York Times). Retrieved 2006-12-03.
- Brousseau, ME; Schaefer EJ; Wolfe ML; Bloedon LT; Digenio AG; Clark RW; Mancuso JP; Rader DJ (April 8, 2004). “Effects of an inhibitor of cholesteryl ester transfer protein on HDL cholesterol” (abstract). New England Journal of Medicine 350 (15): 1505–1515.doi:10.1056/NEJMoa031766. PMID 15071125. Retrieved 2006-12-03.
- http://clinicaltrials.gov/ct2/results?term=torcetrapib
- http://clinicaltrials.gov/ct2/show/NCT00139061 Phase III Assess HDL-C Increase And Non-HDL Lowering Effect Of Torcetrapib/Atorvastatin Vs. Fenofibrate
- http://clinicaltrials.gov/ct2/show/NCT00134511 Phase III Study To Evaluate The Effect Of Torcetrapib/Atorvastatin In Patients With Genetic High Cholesterol Disorder
- http://clinicaltrials.gov/ct2/show/NCT00134485 Phase III Study To Evaluate The Safety And Efficacy Of Torcetrapib/Atorvastatin In Subjects With Familial Hypercholerolemia
- http://clinicaltrials.gov/ct2/show/NCT00134498 Phase III Study Comparing The Efficacy & Safety Of Torcetrapib/Atorvastatin And Atorvastatin In Subjects With High Triglycerides
- http://clinicaltrials.gov/ct2/show/NCT00267254 Phase III Clinical Trial Comparing Torcetrapib/Atorvastatin To Simvastatin In Subjects With High Cholesterol
- http://clinicaltrials.gov/ct2/show/NCT00138762 Phase III Study of Torcetrapib/Atorvastatin vs Atorvastatin Alone or Placebo in Patients With High Cholesterol
- http://clinicaltrials.gov/ct2/show/NCT00134173 Phase III Coronary IVUS Study to Compare Torcetrapib/Atorvastatin to Atorvastatin Alone in Subjects With Coronary Heart Disease (ILLUSTRATE)
- http://clinicaltrials.gov/ct2/show/NCT00137462 Phase III Lipitor Trial To Study The Effect Of Torcetrpib/Atorvastatin To Atorvastatin Alone.
- http://clinicaltrials.gov/ct2/show/NCT00136981 Phase III Carotid B-Mode Ultrasound Study to Compare Anti-Atherosclerotic Effect of Torcetrpib/Atorvastatin to Atorvastatin Alone. (RADIANCE 1)
- Berenson, Alex (December 3, 2006). “Pfizer Ends Studies on Drug for Heart Disease”. The New York Times. Retrieved 2006-12-03.(registration required)
- Theresa Agovino (Associated Press) (December 3, 2006). “Pfizer ends cholesterol drug development”. Yahoo! News. Retrieved 2006-12-03. Each study arm (torcetrapib + atorvastatin vs. atorvastatin alone) had 7500 patients enrolled; 51 deaths were observed in the atorvastatin alone arm, while 82 deaths occurred in the torcetrapib + atorvastatin arm. (Link dead as of 15 January 2007)
- Associated Press (December 2, 2006). “Pfizer cuts off cholesterol drug trials”. Yahoo! News (Yahoo.com). Retrieved 2006-12-03. (Link dead as of 15 January 2007)
- Bots et al.; Visseren, Frank L; Evans, Gregory W; Riley, Ward A; Revkin, James H; Tegeler, Charles H; Shear, Charles L; Duggan, William T et al. (July 2007). “Torcetrapib and carotid intima-media thickness in mixed dyslipidaemia (RADIANCE 2 study): a randomised, double-blind trial”.The Lancet 370 (9582): 153–160. doi:10.1016/S0140-6736(07)61088-5.
- Cutler, D. M. (2007-03-29). “The Demise of the Blockbuster?”. The New England Journal of Medicine (Massachusetts Medical Society) 356 (13): 1292–1293. doi:10.1056/NEJMp078020.ISSN 1533-4406.PMID 17392299. Retrieved 2007-04-23.
External links
Keywords: Antilipemic; CETP Inhibitor; Antiatherosclerotic.

//////////////////////





















No comments:
Post a Comment